The COVID-19 pandemic has caused tremendous upheaval to health systems, disrupting access to family planning information and services. But despite this disruption, the need for family planning remains the same. Family planning is a critical health service that hundreds of millions of women and their partners rely on or want to access. Out of the 923 million women of reproductive age in low- and middle-income countries who want to avoid having a pregnancy, 218 million have an unmet need for modern contraception—that is, they want to avoid a pregnancy but are not using a modern method.
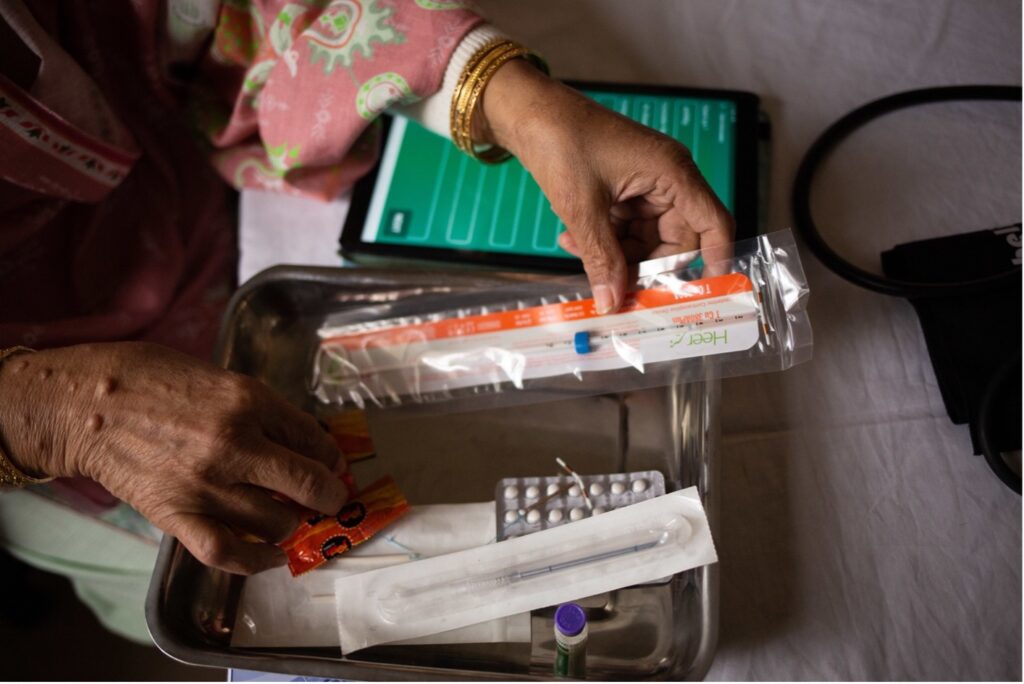
That’s why we have a new vision to transform family planning. Under the leadership of our new family planning and reproductive health director, Dr. Gathari Ndirangu, we will help millions of women access the family planning services they want and need. We plan to do this by integrating family planning with other health and non-healthcare areas; innovating ways to deliver our core strengths more efficiently, effectively and sustainably; striving to offer more and better contraceptive choices through diverse channels of delivery; and leveraging data for decision-making and the private sector to increase impact.
“Our refreshed family planning strategy provides a bold, exciting vision for how Jhpiego can optimize our impact in family planning,” says Megan Christofield, a senior technical advisor for family planning and reproductive health. “Our global team of family planning experts is truly outstanding, and the strategy provides us the scaffolding to increase our impact faster, together.”
Building on a legacy of impact
At Jhpiego, we believe that all people have the right to control when and if they become pregnant. For 50 years, we have worked to transform health care and end preventable deaths. Increasing access to voluntary, informed, rights-based family planning services has been and will always be central to this mission.
Jhpiego has been a longstanding partner in family planning since the 1970s. Our work in family planning began with laparoscopy, which helped voluntary surgical sterilization become safer, simpler and less expensive. It continued with our pioneering efforts in long-acting reversible contraception, including the introduction of new service delivery models, integration with maternal and newborn health, provision of technical guidance and advocacy to expand access to the use of intrauterine contraceptive devices (including postpartum) and contraceptive implants.
Today, Jhpiego offers a diverse set of experiences and expertise spanning clinical settings and service delivery. And, we are expanding access to a variety of methods across the health system, all the way to the community and individual levels.

An integrated approach to delivering health care
Central to Jhpiego’s family planning strategy is the integration of health service delivery within primary health care, which offers a core set of services that can address most health problems in the community, including promotive, preventive, curative and rehabilitative services. Strong and effective primary health care can address 80 percent of people’s health needs across their lifetime. To ensure that all people have access to the health services they need, governments are working with partners like Jhpiego to expand access to primary health care, and within that, access to family planning.
“Family planning is an essential part of primary health care services, but unmet need for family planning remains an urgent priority,” says Chantelle Allen, senior technical advisor, health systems and quality. “As we reimagine how, where and when primary health care services are provided, there are opportunities to bring care closer to people and provide it in the way that they want it, including family planning.”
“In an ideal world, that should be the default,” says Ndirangu. “As long as someone interacts with the health system, they should be able to access the services they need.”
Moving from Data to Action
During the COVID-19 pandemic, many global health programs experienced delays and setbacks in collecting data; however, we know that data can only be used to inform programs if properly collected and analyzed in a timely manner. In three Jhpiego-supported countries implementing family planning programs—Indonesia, Guinea and Kenya—the creation of data dashboards enabled the teams to analyze data in real time, visualize problem areas and quickly offer solutions to improve postpartum family planning services.
Jhpiego is also looking at ways to expand access to family planning services outside of the formal health system, such as from community health workers, drug shops and pharmacies. “We’re really good about integrating family planning with maternal, newborn and child health, but we also need to think about other entry points,” says Ndirangu. “This might require us to step out of the health sector and look at things like where women gather, how we can tap into them and how we better share information and services.”

Expanding partnerships, expanding choice
As we work to better integrate family planning within health and non-health sectors, we are also looking at ways to expand our partnerships with the private sector to enable expanded method choice. In many countries, health care is delivered through mixed health systems—drawing on both the public and private sector to deliver health services. However, in many contexts, full partnership with the private sector to deliver services remains limited. This can be for a variety of reasons, among them challenges with the regulatory environment and financial considerations.
“Finding ways to better engage the private sector as a partner in family planning service delivery has tremendous potential to both expand channels for users to access products and services and provide additional resources for family planning,” says Ndirangu.
“It’s important to impress upon ministries of health that whether people receive their care from the public or private sector, the government is still responsible for peoples’ welfare. When new national guidelines roll out, we must include the private sector. When we talk about quality of care, we must include the private sector. And we need to find ways for the private sector to better feed into national reporting structures.”
Another central issue is the role of private pharmacies in delivering family planning. In most settings, 40 percent of family planning is delivered to people who walk into pharmacies and ask for what they need. “We need to make sure that those who work in pharmacies have the right skills and knowledge to counsel and provide the most appropriate methods, and to be able to refer patients if additional care or counseling is needed,” says Ndirangu.
Newer, self-administered methods, such as DMPA-SC, which is an injectable contraceptive that protects against pregnancy for three months, allow women to take charge of their own health. With these self-care interventions, women are able to independently obtain their method (e.g., from a provider, pharmacy, community-based distributor or virtually) and use it in privacy. As the “go-to” partner of the Ouagadougou Partnership, Jhpiego works in eight Francophone West African countries to introduce and scale-up DMPA-SC.
“By expanding method choice—including not only what people use, but also whether they use family planning and if so, from where—Jhpiego makes quality services and methods accessible to those who want them,” says Christofield.
As governments around the world work to regain progress toward the Sustainable Development Goals, due to setbacks caused by the pandemic, we must redouble our efforts to ensure family planning and reproductive health is prioritized. “It has never been more important to ensure that people have the ability to control whether and when they become pregnant,” says Ndirangu. “It is our hope that together with our partners, our new strategy will help us transform how and where high-quality, voluntary family planning services are accessed.”



