The World Health Organization recommends that all patients who are suspected of having malaria be promptly diagnosed by microscopy or a rapid diagnostic test before being treated.
Year after year, the Tanda Health Center, nestled in the hills of Gicumbi District in the Northern Province of Rwanda, saw a rise in cases of patients suffering from malaria. While there are multiple species of malaria parasites carried by mosquitoes, only one is dominant in Rwanda: Plasmodium falciparum. Because lab technicians were familiar with identifying only one of the species, the Tanda Health Center didn’t have the expertise to identify others and prevent cases of severe malaria in the community.
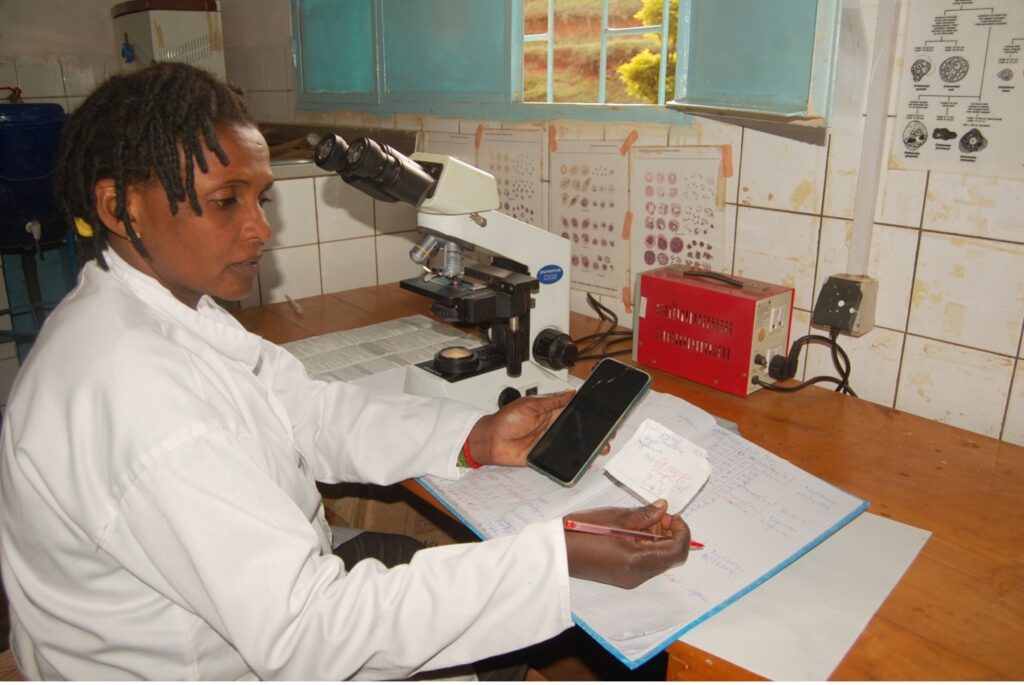
For the last 16 years, Marie Chantal Uwamariya has worked as a lab technician at the Tanda Health Center. As a lab technician, Marie Chantal is responsible for using microscopy to identify malaria parasites in patients’ blood samples. By doing so, she plays a key role in the fight against malaria in Gicumbi District and contributes to the national strategy to reduce malaria-related deaths.
In April 2020, Marie Chantal and 21 other lab technicians from Gicumbi District participated in a malaria microscopy diagnostic training, which was led by the National Reference Laboratory of the Rwanda Biomedical Center and supported by Jhpiego through the U.S. President’s Malaria Initiative (PMI) Impact Malaria project. During the training, participants learned how to differentiate malaria species found in Rwanda and quantify the number of parasites in blood samples, which is essential for accurate diagnosis.

After lab technicians across the country learned to distinguish P. falciparum from uncommon species, the National Reference Lab issued new diagnostic guidelines. When writing up test results, lab technicians are now expected to provide specific details about the malaria parasites identified rather than only giving results as either negative or positive—the parasite is present or not.
The malaria microscopy diagnostic training and updated diagnostic guidelines have enabled lab technicians to improve the quality of diagnostic services in Rwanda, according to Tharcisse Munyaneza, the Senior Parasitology Officer at the National Reference Lab. “We used to think that only the Plasmodium falciparum malaria species was present in Rwanda. Since lab technicians could not identify other species, including Plasmodium malariae, they used to report negative results whenever it was not the species they could identify,” he said.

“After the training, I started differentiating malaria species and the supervision by our trainers from the NRL helped me master the skill. Before the training I found it difficult to tell malaria species apart,” said Marie Chantal. “Plasmodium malariae is difficult to diagnose under a microscope, which can lead to inaccurate results.” Inaccurate results can be a matter of life or death for a patient suffering from malaria.
In the year after the training and with more experience identifying accurate results, Marie Chantal helped save a child who was deathly ill from malaria caused by Plasmodium malariae. Marie Chantal’s accurate diagnosis of the malaria species ensured that the provider could provide timely, proper treatment for the child.
Freddy Turatsinze, the head of Tanda Health Center, said, “Marie Chantal is currently one of the best laboratory technicians who can identify the uncommon species. She provides the National Reference Lab with slides of non-falciparum species that we use as didactic materials for training and supportive supervision.” Freddy noted that better identification of species led to a decrease in cases of severe malaria and hospitalizations.
Currently, with the support of PMI Impact Malaria and the Bill & Melinda Gates Foundation, the Malaria and Other Parasitic Diseases Division of the Rwanda Biomedical Center is carrying out research to establish the prevalence of malaria species and their distribution across the country.
Since 2016, the Jhpiego-led PMI Impact Malaria project in Rwanda has supported the National Reference Lab to train 501 lab technicians from health facilities across the country. This contributed to an increasingly skilled cadre of lab technicians, like Marie Chantal, equipped to provide high-quality malaria diagnostic services. As a result, more patients are getting the right care at the right time.
Globally, PMI Impact Malaria is funded and technically assisted by the U.S. President’s Malaria Initiative (PMI) and is led by Population Services International (PSI) in partnership with Jhpiego, MCD Global Health, and the Malaria Elimination Initiative (MEI) at the University of California, San Francisco.
David Ssekyanzi is the Communications Specialist in the Jhpiego Rwanda office; Noella Umulisa is Jhpiego’s Chief of Party of the PMI Impact Malaria project in Rwanda and was recently elected as the new co-chair of the Roll Back Malaria Case Management Working Group; Jean Modeste Harerimana is a Malaria Technical Advisor in the Jhpiego Rwanda office. Photos by David Sekyanzi.



