These days, when Jenifer Adjei arrives at Oda Hospital, she marvels at the relative peace and quiet that greets her when she walks through the door midday to begin her 12-hour shift as midwife-in-charge.
The number of pregnant women on her labor ward hasn’t decreased; this afternoon she counts 51, a dozen of whom are likely to deliver before her shift ends. But the commotion quotient is markedly diminished here and throughout the facility, compared with months and years past. She attributes this change directly to improved malaria case management as practiced by the nursing and midwifery staff.

Nurses’ and midwives’ competence in implementing malaria rapid diagnostic tests (RDTs) has been a key initiative of the US President’s Malaria Initiative (PMI) Impact Malaria Project to support Ghana’s National Malaria Control Program. Oda Hospital, which serves over 150,000 people living in the Birim Central Municipality of the Eastern Region of Ghana, was prioritized as a high-burden facility that would benefit from malaria case management training.
A midwife since 2008, 30-year-old Adjei is all too familiar with the ravages of malaria, especially how it affects pregnant women and babies. Worldwide, more than 25 million pregnant women are at risk for malaria and 11 percent of all newborn deaths are caused by malaria that occurred in pregnancy. By subscribing to the World Health Organization’s framework for scaling up malaria diagnostic testing, treatment and tracking, Ghana has made substantial gains with malaria-attributable deaths (of all people) declining from 1,565 in 2015 to 249 in 2019. But health facilities serving remote areas often have limited access to good-quality microscopy services and therefore lag in terms of progress. Oda Hospital was among the facilities that reported low adherence to global guidelines for best practices.

During the weeklong training in March 2019, which was led by Jhpiego, Adjei and other hospital department heads identified their facility’s top challenges. Chief among them was a persistent delay in diagnosis and treatment of patients presenting with fever and other symptoms of malaria.
Adjei noted that it wasn’t uncommon for feverish women on the labor ward to languish for several days, growing increasingly sick as they waited on doctors to arrive or for test results to come back, all contributing to chaos, confusion and suffering.
 Learn more from the WHO about what is known about the novel coronavirus, how it spreads and how it is affecting malaria responses worldwide.
Learn more from the WHO about what is known about the novel coronavirus, how it spreads and how it is affecting malaria responses worldwide.
She and others also singled out the non-testing of suspected malaria before treatment, citing countless times when patients with fevers were treated with antimalarials without any prior testing—a dangerous and wasteful practice. It not only increases the risk of antimalarial resistance and fetal loss among pregnant women, but also dips into already constrained pharmaceutical resources.
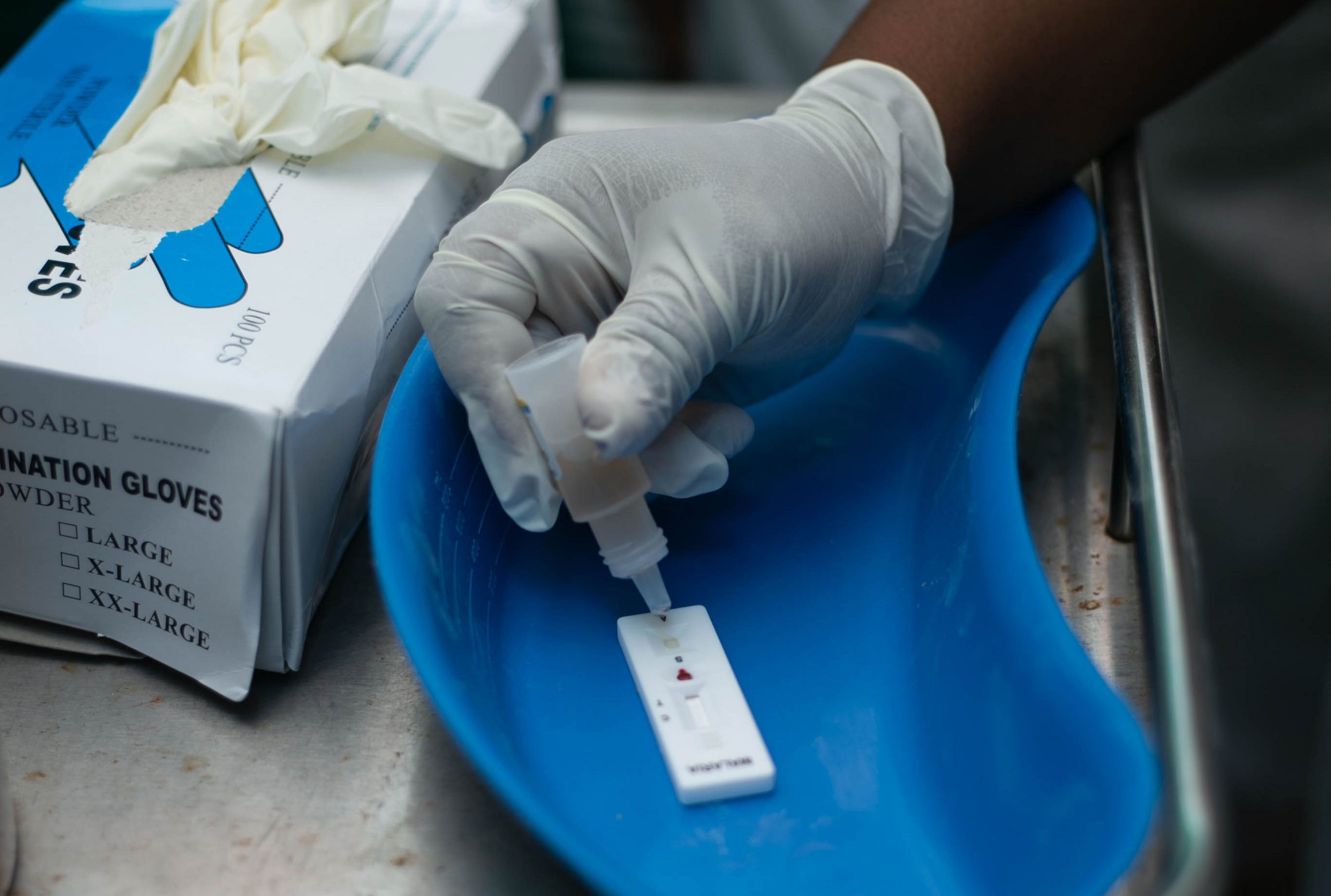
The training directly addressed the shortage of doctors by empowering nurses and midwives to diagnose malaria and, in some cases, treat it. Adjei, for instance, learned how to perform an RDT, calculate a precise dosage and administer proper treatment, whether via injection or pill. She maintains a stock of RDTs on the ward, whereas they previously were available only in the laboratory. RDTs assist in the diagnosis of malaria by quickly detecting evidence of malaria parasites in human blood without having to send a blood sample to a laboratory.
During a series of mentorship visits following the formal training, the Impact Malaria team supported Adjei and her colleagues onsite at Oda Hospital to supervise other providers in the use of RDTs at point-of-care. Subsequently, Adjei led her team of 16 midwives in on-the-job trainings in the outpatient and antenatal care departments and on various wards.
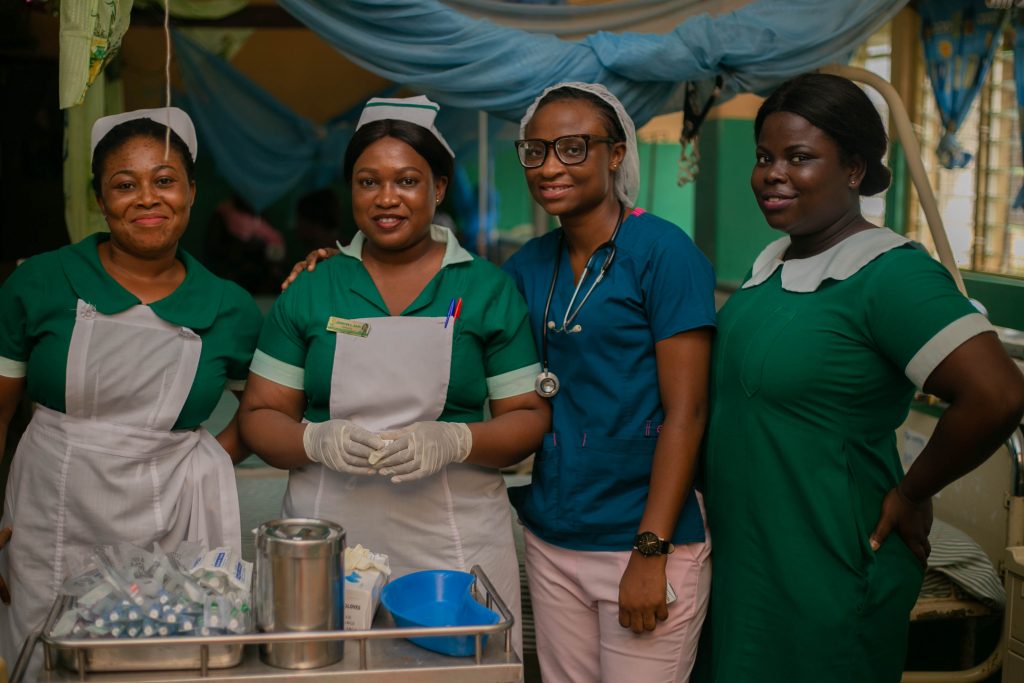
With nurses and midwives able to detect malaria and prescribe and provide holistic care, patients no longer need to wait for days for doctors to manage the process of diagnosis and treatment.
“RDT is simple to perform and provides very quick results,’’ Adjei says. “Patients suffering from severe malaria … spend at most 25 minutes [getting diagnosed].”
Significantly reduced patient wait times and decreased pressure on laboratories allow for overall improved quality of care, Adjei says, noting, “and our antimalarial medicines are now used rationally.”
The presumptive treatment of malaria at Oda Hospital has dropped from 60 percent to zero, which means that every single patient who shows signs of malaria now undergoes microscopy or RDT before treatment. Notably, Oda Hospital has recorded zero malaria deaths from January 2018 through January 2020, according to the Ghana Health Service District Health Information Management System.
Adjei was among 1,200 health workers in 37 high-burden health facilities in Ghana who benefitted in 2019 from Impact Malaria Project-supported malaria case management training by the National Malaria Control Program. With the goal of universal testing of suspected malaria cases, 17,475 health workers in 2,140 health facilities in Ghana are expected to receive Impact Malaria-supported onsite training and supportive supervision.
‘‘Nurses and midwives here are very proud to offer timely relief to the hundreds of patients presenting with symptoms of malaria everyday’’ Adjei says, adding that the emphasis on rapid diagnosis and treatment of malaria frees her up to do what she loves best.
“I really love getting to know my patients, sharing in the awesome moments and supporting them through tough times too.”

Emmanuel Attramah is the knowledge and communications officer for PMI Impact Malaria (IM) Ghana. PMI Impact Malaria is led by Population Services International in partnership with Jhpiego, Medical Care Development International and the Malaria Elimination Initiative at UC San Francisco.
Contributors: Amos Asiedu, Surveillance, monitoring and evaluation advisor, IM Ghana; Pius Affipunguh, regional technical advisor, IM Ghana; Eric LaFary, Peace Corps volunteer; and Anne Bulchis, IM communications manager.



